Effective infection control in clinical settings depends on many small, interlocking practices. One crucial, often overlooked element is the way sterile items are packaged, handled, and maintained between processing and patient use. A well-designed sealed sterilization pouch plays a practical role in reducing opportunities for cross-contamination, protecting both patients and staff while fitting into established sterilization workflows.
The role of packaging in infection prevention begins before a procedure. Packaging preserves the sterility of instruments after they have completed a validated sterilization cycle and until they are opened at the point of use. The Heat Sealing Sterilization Pouch is intended to preserve a sterile barrier through handling, transport, and storage, while allowing staff to see contents and to confirm the pouch integrity prior to use. By maintaining a physical separation between sterilized instruments and the clinical environment, sealed pouches reduce the chance that contaminants will be introduced during routine movement of supplies.
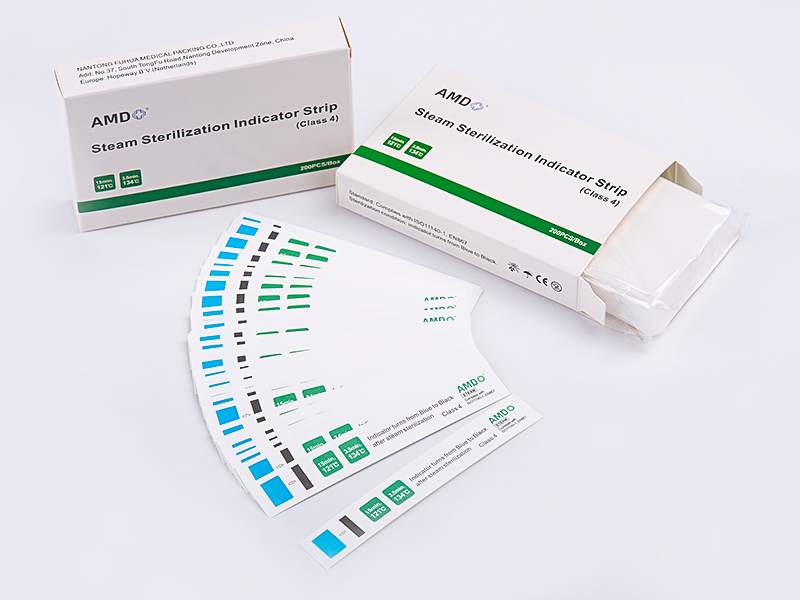
Material selection and package design matter for both function and usability. Packaging must tolerate sterilization conditions without degrading, allow adequate penetration of the sterilant, and provide a reliable seal that resists accidental opening. A pouch that is easy to seal correctly reduces the likelihood of operator error, while clear, consistent sealing indicators help staff confirm that the package has been processed as required. When packaging supports straightforward visual checks and consistent handling, staff can spend less time second-guessing sterility status and more time on direct patient care.
Another practical consideration is the interface between packaging and sterilization equipment. A suitable pouch allows effective exposure to the chosen sterilization method without trapping residual agents or preventing full contact with instrument surfaces. It should also permit safe venting and drying where applicable. Packaging that performs predictably under the conditions used in a facility helps maintain the integrity of sterilization cycles and supports routine monitoring procedures. When the packaging is compatible with the facility's processes, it becomes a reliable component rather than a variable that requires extra oversight.
Human factors also affect how well packaging helps control infection. Clear instructions for sealing, handling, and storage reduce variations in practice. Standard operating procedures that incorporate simple checks — such as inspecting seals and verifying pouch condition before use — make it easier for teams to identify problems before they reach the point of care.
Storage and transport are phases when sterile packaging is particularly vulnerable. Packages that are easy to stack and store while preserving seal integrity store neatly without compromising sterility. Protecting packages from moisture, dust, and physical stress during transport reduces the risk that a sealed pouch will be compromised before it is needed. Where sterile goods move between central sterile processing and clinical areas, clear labeling and careful handling protocols help ensure the package remains intact and identifiable until the moment of opening.
In modern healthcare environments, infection prevention is shaped by a combination of clinical protocols, staff training, and the materials used in daily operations. Among these, sterile packaging plays a quiet but meaningful role. As hospitals refine their processes to balance safety, efficiency, and cost awareness, interest has grown in solutions such as the Heat Sealing Sterilization Pouch, which supports consistent handling of sterilized instruments from processing to point of use.
One of the reasons for this shift lies in evolving expectations around infection control. Healthcare facilities are placing greater emphasis on maintaining a reliable sterile barrier throughout the entire instrument lifecycle. Packaging that can be sealed in a controlled and repeatable manner helps reduce variation in outcomes. When sealing practices are standardized, it becomes easier for staff to follow protocols and verify that instruments remain protected after sterilization. This consistency supports broader infection control strategies without adding unnecessary complexity to workflows.
Another factor influencing adoption is the need for practical cost management. Hospitals operate under ongoing pressure to optimize resource use while maintaining safety standards. Packaging that supports organized storage and efficient handling can contribute to smoother operations. For example, well-structured pouches that are compatible with existing sterilization equipment reduce the likelihood of reprocessing due to packaging issues. Over time, minimizing disruptions in workflow can help facilities manage indirect costs related to labor and material usage.
Ease of use is closely connected to both cost and safety. When packaging is straightforward to seal and inspect, staff can perform their tasks with greater confidence and less ambiguity. Clear visual indicators and a stable sealing process allow for quick checks before instruments are distributed or used. This reduces the chance that compromised packaging goes unnoticed, which is essential in busy clinical environments where time and attention are limited resources.
Material reliability is also a consideration in hospital purchasing decisions. Packaging must withstand sterilization conditions while maintaining its structural integrity during storage and transport. A pouch that holds its seal under routine handling conditions can help prevent accidental exposure of sterile contents. At the same time, it should allow for proper sterilant penetration and release, ensuring that the sterilization process itself is not hindered. When these requirements are met in a balanced way, packaging becomes a dependable part of the sterilization system.
Workflow integration is another important aspect. Hospitals often rely on established sterilization procedures that involve multiple departments, including central sterile processing and clinical units. Packaging that aligns with these workflows helps maintain continuity. For instance, compatibility with labeling systems and ease of documentation can support traceability, making it easier to track instruments from processing to use. This level of organization contributes to accountability and helps facilities respond effectively if questions arise بشأن sterilization records.
The growing attention to environmental responsibility also influences product selection. Hospitals are increasingly aware of the impact of disposable materials and are seeking options that align with waste management policies. Packaging that is designed with thoughtful material use and efficient sizing can support these goals without compromising safety. While infection control remains the priority, aligning packaging choices with broader sustainability considerations reflects a more comprehensive approach to healthcare operations.
In summary, the increasing adoption of sealed sterilization packaging reflects a broader effort to align safety, cost awareness, and operational efficiency. By supporting consistent sealing practices, reliable protection of sterile instruments, and smooth integration into existing workflows, solutions such as the Heat Sealing Sterilization Pouch contribute to a more structured approach to infection control. Hospitals evaluating their options benefit from considering how packaging interacts with daily processes, staff practices, and long-term operational goals rather than focusing on isolated features.
For healthcare providers exploring ways to refine their sterilization workflows, understanding the role of packaging is an important step. Thoughtful selection, combined with clear procedures and ongoing staff engagement, can help create an environment where infection control measures are both practical and sustainable over time.

 English
English Français
Français Deutsch
Deutsch Nederlands
Nederlands












 ‘s-Gravenweg 542, 3065SG RotterdamThe Netherlands
‘s-Gravenweg 542, 3065SG RotterdamThe Netherlands
 +31 (0)10 254 28 08
+31 (0)10 254 28 08







