In sterilization-focused environments, Eo Indicator Strips from Hopeway AMD are part of a practical approach to process verification. For hospitals, laboratories, and medical device manufacturing settings, these strips help users observe whether a package has been exposed to the intended ethylene oxide cycle. They are not a replacement for the sterilization process itself, but they serve as a visual checkpoint within a broader quality routine. As organizations continue to place more attention on consistency, traceability, and workflow clarity, indicator strips remain a familiar tool for supporting those goals.
Content
- 1 What EO Indicator Strips Are
- 2 Their Role in Ethylene Oxide Sterilization
- 3 Why EO Indicator Strips Differ From Steam Indicator Strips
- 4 Why Hospitals Need Them
- 5 Why Laboratories Need Them
- 6 Why Medical Device Factories Need Them
- 7 The Value of Clear Process Visibility
- 8 A Practical Tool for Structured Sterilization Work
What EO Indicator Strips Are
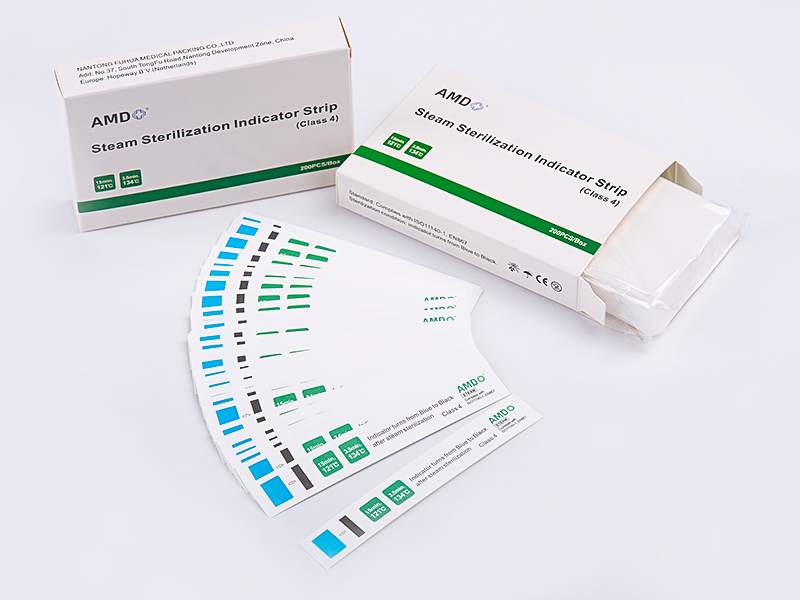
EO indicator strips are designed for use in ethylene oxide sterilization workflows. Their role is straightforward in concept, yet important in practice. When placed inside or alongside packaged items, they respond to the sterilization environment by showing a visible change after exposure to the relevant process conditions. This makes them useful as part of routine verification, especially where packaged instruments, medical supplies, or sensitive materials require careful handling.
The value of these strips lies in their ability to offer immediate visual feedback. In settings where time, organization, and documentation all matter, a simple indicator can help reduce uncertainty. Staff members do not need to infer whether a package has entered the expected process stage. Instead, they can check the strip and use that observation as one part of their review.
That practical function is one reason these strips continue to hold relevance in modern sterilization workflows. They support a methodical approach without introducing complexity. Their presence fits naturally into established procedures, which is important in environments where consistency is preferred over unnecessary change.
EO indicator strips also reflect the broader principle that sterilization is a process of control, not assumption. Packaging, exposure, aeration, and handling all contribute to the final outcome. A strip serves as a visible sign that one stage of the workflow has taken place under the intended conditions. It helps staff maintain a clear separation between unprocessed items and those that have moved through the cycle.
Their Role in Ethylene Oxide Sterilization
Ethylene oxide sterilization is often used for items that cannot tolerate high heat or moisture. Because of that, process monitoring becomes especially important. EO indicator strips fit into this environment by offering a simple way to track whether the package has been exposed to the sterilization cycle. Their function is supportive rather than decisive, but that support matters in daily operations.
In a sterilization setting, every step has a purpose. Materials must be prepared correctly, packaging must remain intact, and the cycle must run according to procedure. Indicator strips help show that the item has reached the phase where exposure to ethylene oxide was intended. That visual confirmation helps staff move through the workflow with greater confidence.
This is particularly useful when handling a range of items at once. Different packages may be prepared for different departments, different procedures, or different storage paths. A clear indicator helps personnel separate completed items from those still waiting for the next stage. That reduces confusion and supports a more orderly workflow.
EO indicator strips also contribute to documentation practices. Even when systems are highly organized, a physical indicator can serve as an additional point of reference. It creates a layer of visible evidence that supports the broader sterilization record. In environments where accountability matters, that kind of clarity is practical.
Another reason they matter is their role in routine checks. Sterilization teams often work under established procedures that leave little room for uncertainty. An indicator strip helps confirm that the package has been processed in the intended way. It becomes part of the everyday language of sterile processing, where simple checks can support reliable routines.
Why EO Indicator Strips Differ From Steam Indicator Strips
EO indicator strips and steam indicator strips may serve similar general purposes, but the sterilization environments they relate to are different. That difference shapes how each one is used, what conditions it monitors, and which types of materials it supports.
Steam indicator strips are associated with moist heat sterilization. They are used in settings where steam is the active sterilizing agent and where materials can tolerate heat and moisture. EO indicator strips, by contrast, are designed for ethylene oxide environments, which are commonly selected for items that are more sensitive to temperature or humidity. This distinction is important because the two processes are not interchangeable.
The physical conditions of each cycle differ significantly. Steam sterilization involves heat and moisture, while EO sterilization relies on a chemical process under controlled conditions. Because of that, the indicators must correspond to the process they are intended to monitor. A strip used for one method is not automatically suitable for the other. Matching the indicator to the sterilization cycle is part of good process management.
Another difference lies in how users think about the materials being sterilized. Steam-compatible items may include instruments and supplies that can handle more demanding thermal conditions. EO-compatible items often include products that require a gentler approach. The indicator strip follows that logic by giving users a process-specific visual cue. It helps prevent confusion between sterilization methods and supports more accurate handling.
The difference is not only technical. It is also operational. In a busy facility, staff members may encounter multiple sterilization methods across departments. Clear separation between EO and steam workflows helps prevent misuse, incorrect identification, or misplaced items. Indicator strips contribute to that separation by making each package easier to interpret at a glance.
For teams managing varied inventory, this distinction has practical value. It supports the right item moving through the right process with fewer delays and less ambiguity. When sterilization tools are aligned with the correct method, workflow quality improves naturally.
| Indicator Type | Sterilization Method | Main Process Condition | Typical Use Scenario | Suitable For |
|---|---|---|---|---|
| EO Indicator Strip | Ethylene oxide sterilization | Low-temperature chemical sterilization | Sensitive medical devices and packaged materials | Hospitals, laboratories, medical device factories |
| Steam Indicator Strip | Steam sterilization | High-temperature moist heat sterilization | Heat-resistant instruments and supplies | Clinics, hospitals, sterilization departments |
| Plasma Indicator Strip | Hydrogen peroxide plasma sterilization | Low-temperature plasma process | Delicate instruments requiring dry sterilization | Surgical centers and specialty departments |
Why Hospitals Need Them
Hospitals rely on organized sterilization practices because patient care depends on predictable handling of instruments and supplies. EO indicator strips fit into that structure by helping staff confirm exposure within the sterilization workflow. In clinical settings, the need for clarity is constant, and anything that reduces uncertainty can support smoother daily operations.
Hospital teams often manage items that vary in shape, sensitivity, and intended use. Some instruments can undergo one sterilization method, while others need another. In that environment, a visible indicator becomes a useful reference. It helps processing staff and clinical teams maintain confidence that items have passed through the appropriate stage before they move forward.
Another reason hospitals use these strips is workflow discipline. Sterile processing departments are built around repeatable steps. A consistent indicator supports those steps by offering a simple visual signal. That signal does not replace procedure, but it complements it. It gives staff one more way to verify that the package has entered the expected process.
Hospitals also value tools that integrate without disruption. Indicator strips do not require major changes to existing systems. They can be used within established packaging and handling practices. That ease of integration is important in a setting where workflows must remain efficient and dependable.
In addition, hospitals often manage high volumes of instruments and supplies. When many packages move through a sterilization cycle, visual indicators help staff sort and review items more efficiently. That supports organization, which in turn supports patient-ready readiness. A clear indicator is a small element that can help maintain a larger system of order.
Why Laboratories Need Them
Laboratories face a different but equally demanding environment. Their work often involves instruments, containers, or materials that must be processed carefully before reuse or handling. EO indicator strips offer a practical way to show that a package has been exposed to the intended sterilization cycle without interrupting the laboratory workflow.
Lab environments are known for precision. Procedures must be followed carefully, and materials often move through tightly managed stages. In that context, a simple visual indicator can support better oversight. It allows staff to distinguish between items that are ready for the next step and those that still require processing.
Laboratories also handle a wide range of equipment types. Some materials may be too delicate for high heat or moisture, making EO sterilization the more suitable option. That is where process-specific indicators matter. They help the lab maintain a clear relationship between the sterilization method and the material being processed.
A laboratory may also need to manage shared equipment across different projects or teams. When several users rely on the same instruments, clear marking and confirmation become even more important. Indicator strips help maintain that clarity. They serve as a reference point that supports both organization and confidence.
Because laboratory work often involves recurring routines, tools that reduce ambiguity are especially useful. EO indicator strips provide that type of support. They are simple, visible, and easy to incorporate into standard practice. In an environment where attention to detail is part of the daily rhythm, that matters.
Why Medical Device Factories Need Them
Medical device factories operate under a different kind of pressure. Their focus is on production, quality control, packaging integrity, and consistent process management. EO indicator strips fit into that structure because they help show that an item or package has been exposed to the intended sterilization cycle before it moves into the next stage.
Manufacturing environments depend on repeatable systems. Every component, package, and workflow step must align with internal standards and external expectations. A visible indicator helps maintain that alignment. It supports the transition from production to sterilization review, and then toward storage or distribution.
In factories, traceability is especially important. When items move through multiple stages, the ability to identify processed packages quickly becomes useful. Indicator strips provide a straightforward visual cue that supports that process. They help personnel organize batches, manage quality review, and maintain workflow discipline.
Another reason factories rely on these strips is product variety. Medical devices may differ in shape, material sensitivity, and sterilization requirements. EO is often chosen for items that need a gentler process than steam can provide. A corresponding indicator helps confirm that the correct sterilization route has been used. That reduces confusion and supports process accuracy.
Factories also benefit from solutions that are easy to scale within existing operations. Indicator strips do not complicate production lines. They fit into packaging and verification steps without demanding large procedural changes. That makes them a practical option in settings where efficiency and consistency must work together.
The Value of Clear Process Visibility
Across hospitals, laboratories, and manufacturing facilities, one theme remains constant: people need to know where an item is in the sterilization workflow. EO indicator strips help provide that visibility. They make an invisible process easier to track through a visible signal, and that makes everyday handling more manageable.
This kind of visibility supports better communication among teams. When one group prepares a package and another reviews it later, a shared visual cue helps reduce misunderstanding. It gives everyone involved a common reference point. That matters in environments where many people are responsible for different parts of the same workflow.
Clear visibility also supports routine discipline. A process that can be checked easily is more likely to be followed carefully. Indicator strips contribute to that structure by making verification part of the normal handling pattern. They help turn sterilization from an abstract expectation into a visible step.
In practice, that means more organized processing, fewer questions during review, and a smoother path from preparation to use. While the strip itself is simple, its role in the larger system is meaningful. It helps keep attention on the details that matter.
A Practical Tool for Structured Sterilization Work
EO indicator strips continue to play a useful role because they fit into the real conditions of medical, laboratory, and manufacturing work. They do not ask users to change the system. They support the system already in place. That makes them a practical choice for teams that value clarity, routine, and process alignment.
Their value is found in what they help confirm. They offer a visible sign within a chemical sterilization workflow, helping staff make informed decisions about handling and readiness. They distinguish EO processes from steam-based methods, which is important when different sterilization routes are used in the same organization.
For institutions that depend on organized workflows, that kind of support matters every day. It is one more way to keep sterilization visible, manageable, and connected to the responsibilities of the people who rely on it.
A process can be complex without needing to feel unclear. When teams have tools that fit the method they use, the workflow becomes easier to trust.

 English
English Français
Français Deutsch
Deutsch Nederlands
Nederlands












 ‘s-Gravenweg 542, 3065SG RotterdamThe Netherlands
‘s-Gravenweg 542, 3065SG RotterdamThe Netherlands
 +31 (0)10 254 28 08
+31 (0)10 254 28 08







