Medical sterilization packaging has changed with the way healthcare works. As clinics, hospitals, dental practices, and laboratories continue to refine their infection control routines, packaging is no longer viewed as a simple outer layer. It is now part of a broader system that supports cleanliness, workflow, traceability, and product handling from preparation to point of use.
Among the packaging formats that remain widely discussed, flat roll structures continue to attract attention because they offer a practical balance of form, use, and storage. In this context, Sterilization Flat Roll is often associated with a market segment that focuses on consistency, seal integrity, and compatibility with common sterilization processes.
Content
- 1 From basic wrapping to controlled packaging
- 2 Why material choice matters more now
- 3 The growing role of indicators and visibility
- 4 The place of packaging in hospital infection control
- 5 Reducing cross-contact through controlled presentation
- 6 Why hospitals pay attention to packaging materials
- 7 A practical role that remains important
From basic wrapping to controlled packaging
The early stage of medical sterilization packaging was shaped by a simple goal: keep contents protected until use. Over time, that goal expanded. Healthcare facilities began to consider how packaging interacts with heat, moisture, gas, handling, transport, and shelf storage. This shift helped move the category from basic wrapping materials toward more structured and standardized formats.
Today, healthcare users expect packaging materials to support several tasks at once. They need a clear barrier against contamination. They need packaging that can be handled without unnecessary difficulty. They need materials that work with established sterilization methods. They also need a format that fits routine operations without forcing major changes to existing equipment or training.
Flat roll packaging became relevant in this setting because it can be adapted to different item sizes and pack configurations. That flexibility matters in clinical environments where instruments vary from one department to another. Instead of relying on a narrow set of pre-made sizes, users can prepare packages that match the item more closely. This can help reduce waste and support orderly inventory use.
Why material choice matters more now
Material selection has become a central topic in sterilization packaging because the healthcare sector is paying closer attention to resource use and operational consistency. Buyers are no longer focused only on whether a package can be sealed and sterilized. They also want to know how the material behaves during storage, how clearly it can support inspection, and how well it fits current procurement standards.
Paper-film combinations remain widely discussed in this field because they offer a familiar structure with a visible transparent side and a breathable side. This type of construction supports inspection and sterilization workflows while giving users a way to view the contents after sealing. At the same time, manufacturers are looking at material development from another angle: reducing excess material use and improving compatibility with responsible supply-chain choices.
Environmental considerations are becoming part of the conversation. Healthcare organizations are increasingly interested in packaging that aligns with internal sustainability goals without disrupting sterility management. That does not mean every product must change overnight. It does mean that future packaging development will likely be shaped by material efficiency, sourcing awareness, and waste reduction methods that can be adopted gradually.
The growing role of indicators and visibility
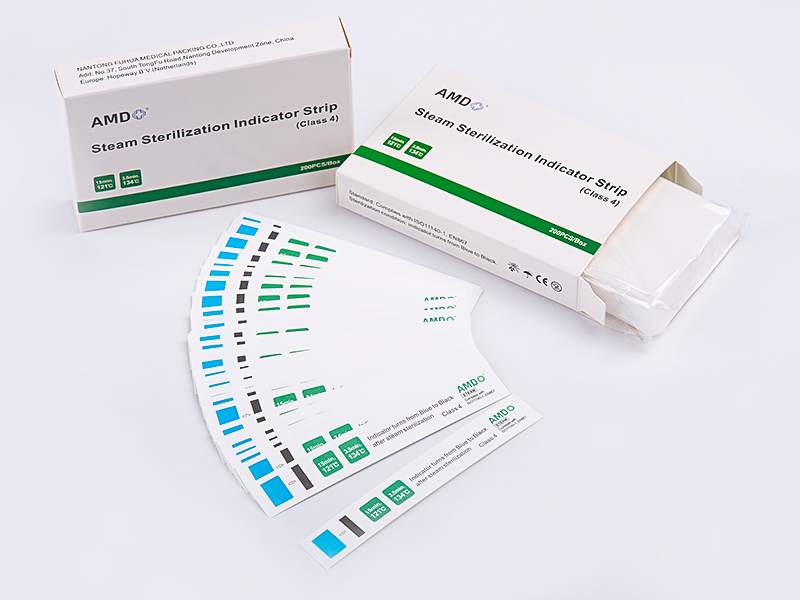
One of the notable directions in sterilization packaging is the movement toward clearer process visibility. Healthcare users want packaging that not only protects an item, but also provides meaningful visual cues during sterilization and storage. This is where smart indicators and improved marking systems become relevant.
Traditional indicators already help users confirm that a package has been exposed to a sterilization process. Future development may take this a step further through more readable indicators, more stable color response, and better distinction between processed and unprocessed items. In busy environments, those small improvements can support smoother handling and reduce uncertainty during sorting and distribution.
Visibility also matters in a practical sense. Transparent film sections allow staff to inspect item placement and confirm whether a pack is arranged properly before use. This kind of visual support is valuable in departments where speed and accuracy both matter. As packaging evolves, clearer inspection windows and more stable indicator placement may become standard expectations rather than optional features.
The place of packaging in hospital infection control
Hospital infection control is shaped by a chain of small decisions. Cleaning, disinfection, sterilization, packing, storage, transport, and point-of-use opening all contribute to the final outcome. If one part of the chain is handled poorly, the entire process may become harder to manage.
Packaging sits between sterilization and clinical use. It helps preserve the condition of the item after the sterilization cycle is complete. In that sense, packaging is not a passive layer. It is part of the control process itself. It gives hospital staff a way to keep processed instruments identified, contained, and protected during handling.
This is especially important in places where many people work with shared supplies. Operating rooms, dental departments, emergency units, wards, and procedure rooms all depend on orderly instrument flow. The more clearly a sterile item is packaged and labeled, the easier it is for staff to move it through the system without confusion.
| Infection Control Step | Function of Sterilization Packaging | Practical Outcome in Hospitals |
|---|---|---|
| Post-Sterilization Protection | Maintains barrier after sterilization process | Helps keep instruments isolated from exposure |
| Storage Management | Organizes sterile items in controlled conditions | Reduces mix-up between sterile and non-sterile items |
| Handling and Distribution | Supports safe transport within departments | Limits unnecessary contact during movement |
| Visual Inspection | Allows quick check of package condition | Helps identify damaged or compromised packs |
Reducing cross-contact through controlled presentation
Cross-infection concerns often begin when sterile and non-sterile items are not clearly separated. Packaging helps create that separation. A well-structured sterile package supports a clear boundary between the item and the surrounding environment. That boundary matters during storage, transport, and opening.
Flat roll packaging offers flexibility because it can be sized according to the item being packed. This helps reduce unnecessary extra space and gives staff a more tailored packaging option. When the package matches the contents more closely, it can support tidier storage and easier handling. A neat, controlled package is less likely to be disturbed during movement and easier for staff to inspect before use.
The process of opening also matters. In clinical practice, the opening of a sterile package should be handled in a way that keeps the contents ready for use without adding avoidable contact. Packaging that is stable and clearly formed can help support that workflow. It gives staff a predictable structure to work with, which is useful in busy departments where time and attention are often divided across several tasks.
Why hospitals pay attention to packaging materials
Hospitals and clinics often evaluate packaging not just by appearance, but by how well it fits daily work. Materials need to be usable, stable, and compatible with existing sterilization and storage practices. If packaging is difficult to handle, it can slow the workflow. If it is too limited in format, it may not suit different instrument sizes. If it does not support proper sealing and storage, it may create avoidable complications.
This is why packaging materials remain a practical concern for procurement teams and sterile processing departments. They are looking for materials that fit their environment, their equipment, and their handling routines. In infection control, small details matter. A dependable packaging format can make those details easier to manage.
Sterilization Flat Roll is one example of a packaging approach that fits this operational mindset. It offers a usable format for item-specific preparation, while Hopeway AMD reflects how brands are positioned in a market that values consistency and controlled presentation. The discussion is not about dramatic claims. It is about practical support for a hospital's infection control routine.
A practical role that remains important
The role of sterile packaging is often understated because it works behind the scenes. Yet infection control depends on reliable behind-the-scenes systems. When sterile items are packed, stored, and opened in a controlled manner, the hospital gains a more orderly process and a clearer path from sterilization to patient care.
That is why packaging continues to hold an important place in clinical operations. It helps reduce unnecessary exposure, supports better handling discipline, and gives staff a more dependable way to manage sterile supplies. In a healthcare environment where every step is part of a larger safety chain, this kind of support matters.
Sterile packaging will continue to evolve, but its basic purpose remains steady: to help keep processed instruments in a controlled state until they are ready to be used. For hospitals focused on infection control, that purpose is both practical and essential.
As healthcare organizations continue refining their internal standards, sterile packaging will remain part of the conversation about safety, process order, and handling discipline. Its contribution may be quiet, but it is consistent. By supporting clear separation, careful storage, and controlled opening, it helps strengthen the everyday routines that hospital infection control depends on.

 English
English Français
Français Deutsch
Deutsch Nederlands
Nederlands












 ‘s-Gravenweg 542, 3065SG RotterdamThe Netherlands
‘s-Gravenweg 542, 3065SG RotterdamThe Netherlands
 +31 (0)10 254 28 08
+31 (0)10 254 28 08







